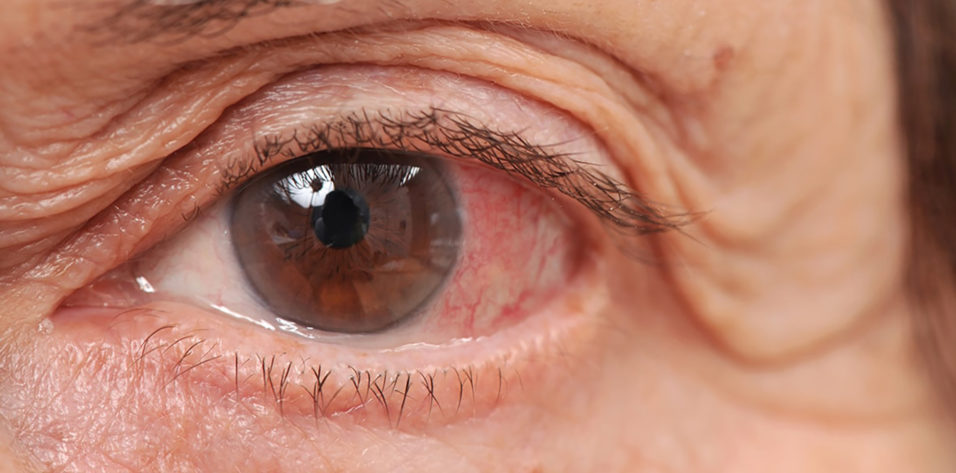
Every medically minded optometrist who comanages surgical patients knows the importance of managing ocular surface disease (OSD), blepharitis, and other factors that could potentially complicate a procedure and affect its outcome before referring a patient for penetrating ocular surgery. Doing so can reduce the chances of postoperative complications.
Communication plays a key role, both between the comanaging optometrist and the surgeon and between the optometrist and the patient. In your referral notes, be sure to alert the surgeon to conditions that could have an impact on surgical planning and techniques and, ultimately, results: for example, a chronic blepharitis or keratitis that has required ongoing treatments. That way, the surgeon knows to take extra caution preoperatively or intraoperatively. Likewise, educating the patient about what to expect in terms of medications and follow-up will go a long way toward setting expectations and establishing trust.
In this article I review five common complications optometrists may encounter while comanaging patients after penetrating ocular surgery (eg, retinal surgery, glaucoma surgery, corneal transplants, cataract surgery).
NO. 1: ENDOPHTHALMITIS
After any ocular surgery that involves entering the eye, the most concerning complication is a postoperative infection inside the eye (endophthalmitis), which typically develops in the days or weeks after surgery.1 Although the incidence of endophthalmitis after ocular surgery is relatively low (0.03% to 0.68%, depending on the type of surgery), it’s probably the most concerning complication because of the potential for the patient to permanently lose vision and even lose the eye itself.
Diagnosis
At any postoperative visit, make sure the patient is not showing early signs of endophthalmitis, which would include a swollen eyelid, decreasing vision, increasing pain, hypopyon, vitreous inflammation, and corneal edema.
Management
If you are concerned about endophthalmitis, communicate with the primary surgeon immediately by phone. Because this is the most concerning postoperative complication, rapid referral to the correct specialist—usually a retina specialist—is critical. Even if you send the patient back to the operating surgeon, in most instances that surgeon will send the patient to see a retina surgeon for fortified antibiotics, tapping and culturing, and possible surgical intervention. In some cases the retina surgeon will treat the patient even before obtaining culturing results.
Prevention
Risk factors include OSD; active infections, including eyelid; and blepharitis. Therefore, make sure you address the patient’s ocular surface before referral. Significant OSD can harbor pathogens that can find their way into the eye during or after surgery through the surgical wounds. Prophylactic use of a topical antibiotic is a popular tactic, and most surgeons start such drops before surgery. Some will also inject antibiotics directly into the eye before the end of a case.
NO. 2: INFLAMMATION
The most common complication associated with any kind of penetrating ocular surgery is inflammation, which is due to the breakdown of the blood-aqueous barrier inside the eye during surgery. If there’s an insult to the blood-aqueous barrier, there will be inflammation inside the eye.
Diagnosis
Patients may complain of light sensitivity, soreness, blurred vision, redness, or tearing. These are very common symptoms even after uncomplicated ocular surgery.
Prevention
There is a prevailing thought that preoperative prophylactic use of a nonsteroidal antiinflammatory drug (NSAID) and in some cases a steroid in the days before surgery can reduce the inflammatory response. These drops are then continued through the postoperative period. Some surgeons inject steroids intraoperatively or insert intracanalicular plugs that deliver steroids to the surface of the eye on a consistent basis during the postoperative period. Regardless of mode, antiinflammatory therapy is essential.
Management
Proper use of a topical antiinflammatory drug preoperatively and postoperatively is typically enough to manage the inflammation. There are a number of steroidal and NSAID options, and you may find it necessary to change drops or dosing regimens if your patient doesn’t respond well to your first choice. In my experience, patients with comorbidities (eg, diabetes, systemic inflammatory disease, etc.) are prone to heavier inflammation, so you may want to watch them more closely and either extend the drop regimen or increase the frequency of drops.
One should also be aware of the risk of rebound inflammation, which typically occurs within a few weeks of the patient ceasing their medications. In extreme cases, you might confuse the symptoms with endophthalmitis, but careful examination can usually make the delineation clear. Again, it may be necessary to change medications or dosing schedules at that point.
Postoperative inflammation is very much in the wheelhouse of optometrists to manage. If you find that, with a certain subset of surgeons or surgeries, inflammation is beyond what you would expect as normal, it’s important to communicate this to the surgeon. This information makes him or her aware of the issue and may prompt modification of surgical techniques (eg, things that are done prophylactically before surgery or during the surgery) that can lead to better results for future patients. The same is true for all of the complications discussed here. Surgeons appreciate the feedback as they track their results.
TASS
Toxic anterior segment syndrome (TASS) is a subset of inflammation. TASS is a rare but severe inflammatory reaction, above and beyond normal postoperative inflammation, that can occur within hours to days after surgery.2 It is a noninfectious process and is thought to be a reaction to some kind of foreign substance or debris introduced into the eye during surgery or shortly afterwards.
TASS creates a significant inflammatory episode that can be confused with endophthalmitis. In most cases, TASS is not painful, unlike endophthalmitis, even though the symptoms are similar (eg, decreased vision, corneal edema, and significant anterior chamber reaction, maybe even with a hypopyon). It also tends to develop rapidly and not to involve the vitreous. Patients with TASS respond well to aggressive use of antiinflammatory therapy.
If you are concerned that a patient may have endophthalmitis rather than TASS, it’s best to err on the side of caution and refer him or her back to the primary surgeon or to a retina specialist to be sure.
NO. 3: CORNEAL ABRASIONS
Corneal abrasions are a common complication of penetrating ocular surgeries, as many of the instruments used (eg, lid speculums and scalpels) can disrupt the corneal epithelium. Additionally, many of the drops, including anesthetics and antibiotics used preoperatively and intraoperatively, can irritate the cornea and increase the likelihood of an abrasion. The frequent application and preservatives might play a role in this scenario. Top that off with the fact that patients may have a history of recurrent corneal erosion (RCE) or epithelial basement membrane dystrophy (EBMD), putting them at increased risk for corneal abrasion with any kind of surgery.
Prevention
Preoperatively, even before the patient is sent to the surgeon, it’s imperative to look for conditions such as EBMD, RCE, or significant OSD that may compromise the cornea. If you see any of these conditions, manage them before the patient sees the surgeon and don’t forget to mention them in your referral notes.
Management
Optometrists are well-equipped to manage corneal abrasions. Whether you see these patients at postoperative day 1, day 3, or week 1, many can be managed topically with heavy use of lubricant eye drops or ointments and decent rest. Let the patient know to expect some irritation for the first few days.
Depending on the size and extent of the abrasion, the use of a bandage contact lens or amniotic membrane may be required to help keep the patient comfortable. He or she may complain about either blurry vision or significant discomfort or foreign body sensation.
Rarely do patients with corneal abrasions have to be returned to the surgeon. Even in cases of neurotrophic keratitis, we now have the potential to manage these with cenegermin-bkbj ophthalmic solution 0.002% (Oxervate, Dompe Pharmaceuticals).
NO. 4: HYPHEMA
With the advent of microinvasive glaucoma surgery (MIGS), we may now encounter patients with hyphema postoperatively. These complications don’t occur commonly, and when they do they tend to be small microhyphemas that cannot be seen grossly at the slit lamp without the use of a goniolens or gonioscopy.
Management
Whether a hyphema is related to MIGS or another type of penetrating ocular surgery, most will resolve with proper management. Instruct the patient to keep his or her head elevated, and treat comorbidities such as inflammation and elevated IOP. Rarely will a patient need to be referred back to the surgeon, unless the hyphema is so large or nonresolving as to warrant an anterior chamber washout. Be sure to let the patient know that this issue will resolve with proper treatment, in order to reduce anxiety.
NO. 5: PTOSIS
Ptosis is one of the underreported complications of ocular surgery. Informed consent often focuses on infections and bleeding, but some will mention the risk of postoperative ptosis. Sometimes the eyelid droops after surgery due to lid edema, small hematomas, or bruising. Other potential causes may include use of the lid speculum or anesthesia myotoxicity.3
Management
In most cases, ptosis will self-resolve. Be patient and understanding when you inform patients of this. Let them know that if it doesn’t resolve, or if they are unhappy with the cosmetic results, there are treatment options. Aside from blepharoplasty, there now exists a nonsurgical option: oxymetazoline HCl ophthalmic solution 0.1% (Upneeq, RVL Pharmaceuticals). This drop is available by prescription via a mail-order pharmacy, and I have found it to be very successful in helping lift ptotic lids.
Most of the time, however, you just need to do a little coaching and handholding, and patients don’t have to be referred back to the surgeon. If the ptosis is not resolved to the patient’s liking, and if oxymetazoline isn’t successful or is not an option, then referral to an oculoplastics specialist for blepharoplasty is always an option.
COMMUNICATION IS KEY TO MANAGEMENT
Most of the complications discussed here can be managed by the referring optometrist in the office. It is important, however, to establish and maintain communication with your patients’ primary surgeons about both complications and good outcomes so that they can track their results. Many surgeons want to look for trends in their results and will make adjustments for future surgical patients if they’re not getting the outcomes they expect. If the surgeon you’re working with isn’t willing to engage with you regarding postoperative information, I would advise finding a different surgeon to work with.
1. Kamjoo S. Endophthalmitis.American Academy of Ophthalmology. eyewiki.aao.org/Endophthalmitis Accessed March 22, 2021.
2. Park CY, Lee JK, Chuck RS. Toxic anterior segment syndrome-an updated review. BMC Ophthalmol. 2018;18:276.
3. Passut J. Post-surgical ptosis: causes and treatments. EyeWorld. November 2012. www.eyeworld.org/article-post-surgical-ptosis. Accessed March 10, 2021.