The number of diabetic patients we see in our clinics today is nothing compared to the numbers we will see in the future. The 2017 Diabetes Statistics Report revealed some alarming numbers. There are 30.3 million individuals with diabetes in the United States (9.4% of the population), but only 23.1 million of them are diagnosed. This leaves 9.0 million people with undiagnosed diabetes.1
Even more noteworthy, there are 84.1 million people with prediabetes.1 If these people are not identified and treated, they will likely develop type 2 diabetes within 5 years.1
As these statistics show, with almost 330 million people in the United States today, approximately one of every three people in this country has either diabetes or prediabetes. The earlier we can detect this disease, the better the outcomes for our patients.
However, there is a challenge to identifying patients with prediabetes. Simply put, the health care system is overtaxed. Primary care physicians and endocrinologists are already struggling to deal with patients who are diagnosed with the disease.
Other Challenges
Many times, when patients with prediabetes have routine physicals, they are not tested for diabetes unless they report symptoms, are obese, have a family history, or express a desire to be tested. And often, when patients are diagnosed with prediabetes during a physical exam, their physicians are so rushed that they have time for only minimal discussion, which typically amounts to advising patients to watch their diet, exercise, and try to lose a few pounds. With so many patients with diagnosed diabetes to monitor, there is little time left to worry about those with prediabetes.
When patients with undiagnosed diabetes and those with prediabetes come to us for vision care, technicians may gather inaccurate information when taking the physical history. This is because both patient types are usually unaware of their condition, and they may respond negatively to queries about diabetes. Such patients are often in denial or downplay the significance of their condition. They may tell the technician that they don’t have a blood sugar problem or that their doctor said that they only needed to change their diet.

A KEY QUESTION
Whatever the scenario, with an inadequate history, we don’t realize that these patients are diabetic or on the verge of becoming diabetic, which leads to a dilemma for the eye care provider. If the patient doesn’t know that he or she is diabetic or prediabetic and has no obvious diabetic retinopathy, how do we make these diagnoses?
ENTER ELECTRODIAGNOSTICS
Visual electrodiagnostic testing can help eye care practitioners detect visual function changes, assess disease severity, and tweak patients’ treatment plans. Several forms of electrodiagnostic testing are detailed in Visual Electrodiagnostic Testing Options.
Electroretinography (ERG) is a diagnostic test modality that measures the responses of cells in the retina to light stimuli. Flicker ERG, a specific form of ERG using flicker stimuli generated by a mini Ganzfeld device (fixed or multiluminance), can be used to detect whether patients with diabetic retinopathy are at risk for developing neovascular changes. Could ERG also be used to uncover at-risk patients with prediabetes or undiagnosed disease?
Flicker ERG is an objective, frequency-domain–based test that gathers many responses in a short period of time, samples the entire retina, and is accurate in its assessment of the retina. In order to justify reimbursement for use of this technology, however, the patient being tested must have documented retinal vascular changes (ie, a CPT code description on record).
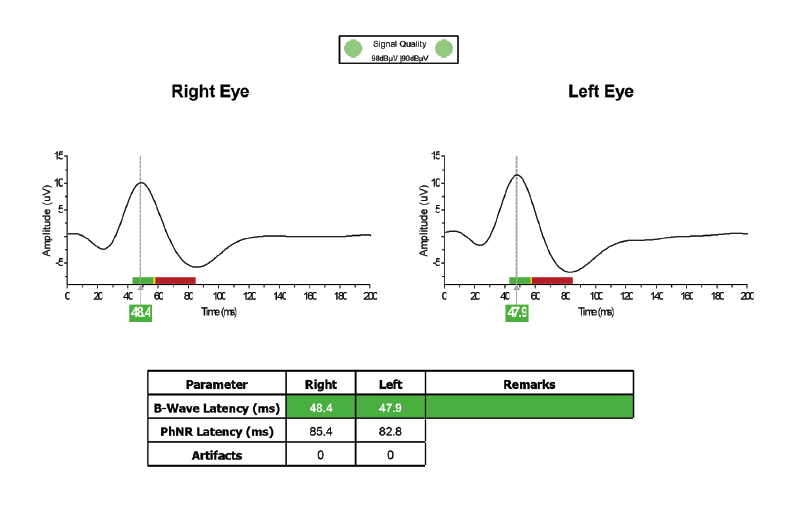
Figure. Example readout of a normal Diopsys Chromatic Flash Vision Screener test.
Patients with prediabetes and many patients with undiagnosed disease obviously do not meet this criterion. This led to the creation of the Diopsys Chromatic Flash Vision Screener (CFVS; Diopsys), an add-on to the existing Diopsys full field ERG module.
The CFVS module uses time-domain technology rather than frequency-domain, which allows a much larger sample size and more advanced algorithms. Used as a screening test, the CFVS requires only time-domain analysis.
Because the CFVS is a screening device, it is not reimbursed by insurance, so patients must pay out-of-pocket for the testing. The test and associated fee can be introduced to patients at check-in or discussed with them during examination. It is important to note that, in a busy practice, if you introduce patients to the CFVS at check-in, they may expect to be tested during the visit, which could create congestion in patient flow.
Interpretation of the CFVS test is simple and quick, making it something worth sharing with the patient’s primary care physician or endocrinologist to let them know which patients may need more monitoring and which are doing fine.
When looking at the test result (Figure), first determine whether the signal strength is green, then find the line intercepting the B wave peak and follow it down to where it intersects the latency values. These values will be green, yellow, or red, indicating within range, borderline, and out of range, respectively. Latency values are not necessarily static. If a patient with an abnormal CFVS result becomes involved in controlling his or her plasma blood sugar levels, it is not unusual to see the abnormal values become less abnormal, or even normal, reflecting improvement.
EARLY DETECTION: A STEP IN THE RIGHT DIRECTION
Although we can’t control the growing numbers of patients with diabetes and prediabetes who will be heading to our offices, there is now an affordable and easy-to-use diagnostic technology to identify patients who are at risk and help them get control of their disease before complications arise or worsen.
- National diabetes statistics report, 2017: estimates of diabetes and its burden in the United States. Centers for Disease Control and Prevention. www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf. Accessed May 20, 2019.




