The changing landscape in eye care calls on optometrists to take a leading role in medical diagnosis and treatment—a shift that’s now driving high growth in our profession, aided by an aging population. While comanagement for surgery and glaucoma command a lot of the discussion, dry eye disease (DED) stands out as both a primary focus and a component of other problems.
The biggest challenge of DED continues to be underdiagnosis. Even as objective point-of-care testing such as osmolarity/salt concentration, MMP-9, and meibography are added to standardized dry eye screening questionnaires, staining, and tear break-up time to offer a complete diagnostic picture, most patients with DED are still not diagnosed. Knowing that this is a chronic, progressive disease, optometrists have a responsibility to catch and treat DED and prevent permanent damage.
How Much Data Do You Need?
I mentioned objective testing for DED, which I find helps me to diagnose the problem in detail. However, you don’t need to have a lot of devices to make a basic diagnosis. In fact, given the problem with underdiagnosis, it’s essential that we all diagnose DED, regardless of the technology at our disposal.
A standardized dry eye questionnaire and face-to-face questions go a long way. Alcon data show that of the 30 million Americans with dry eye,1 72% treat it themselves with over-the-counter drops,2 so asking if patients use artificial tears is a good starting point for discussion. The answers lead to a more in-depth examination of the tear film and meibomian glands, and perhaps a look at tear break-up time and staining. In most cases, for a basic diagnosis, that may be all the data you need.
Also be aware that the patient might have aqueous-deficient or evaporative dry eye or both. About 86% of dry eye has a component of evaporative disease,3 or meibomian gland dysfunction. There are a lot of effective treatments for DED today, but all of them will include artificial tears, and the prevalence of meibomian gland dysfunction makes it important for those tears to address the lipid layer as well as adding moisture.
Can One Drop Treat Everyone?
Although about 86% of dry eye patients have at least some evaporative component, I’d estimate that only about 15% of over-the-counter tears are lipid-based. And when practitioners don’t specify which over-the-counter tear patients should use, odds are that patients purchase tears that fall into that other 85% that only address aqueous deficiency. I make a specific written recommendation, and our staff delivers a consistent message as well: advanced technology tears will help protect the ocular surface and alleviate DED.
I’ve been recommending SYSTANE COMPLETE artificial tears since they became available in March, and the strongest praise I can relay to other optometrists who want to take on the widespread problem of DED is that these tears simplify treatment. Before this drop, we had to choose between an aqueous or lipid-based tear. SYSTANE COMPLETE is designed to provide symptom relief for every major type of dry eye,4-6 combining systematic and sustained relief in stabilizing tears7—it’s one simple choice for dry eye.
SYSTANE COMPLETE is different from other drops in several ways. It has a high concentration of a gelling agent called hydroxypropyl-guar (three times the concentration of SYSTANE BALANCE Lubricant Eye Drops). When the drop is instilled, it creates a mesh-like network that provides better coverage of the ocular surface compared to SYSTANE BALANCE,4,5 fast-acting hydration, and long-lasting relief (Figure 1).4,5,7-10 The drops also contain a phospholipid to support all layers of the tear film11-13 and provide tear evaporation protection.8 The components of SYSTANE COMPLETE are able to reach the ocular surface, create this meshwork, and minimize blur because of their smaller particle size,14 which provides better coverage of the ocular surface compared to SYSTANE BALANCE Lubricant Eye Drops,4,5 and supports all layers of the tear film.11-13
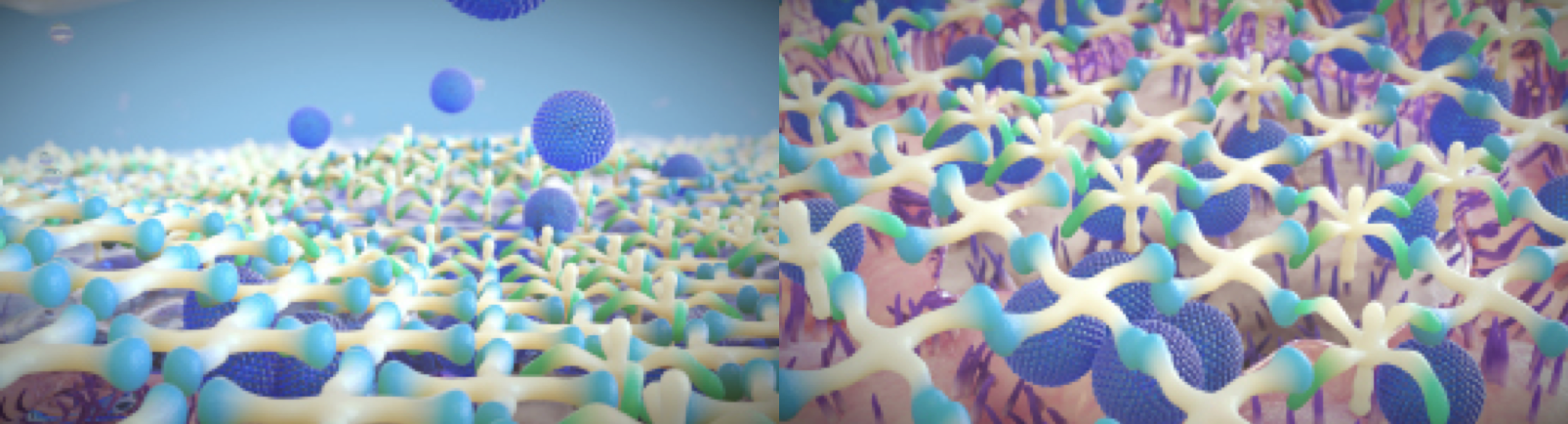
Figure 1. When the drop is instilled, it creates a mesh-like network that provides better coverage of the ocular surface compared to SYSTANE BALANCE,4,5 fast-acting hydration, and long-lasting relief.4,5,7-10
What Do Patients Say?
I received great feedback on SYSTANE COMPLETE very quickly from my patients, who noted they felt more soothed and the effects lasted longer. I recently gave the tears to a longtime dry eye sufferer who has had punctal occlusion, uses a prescription anti-inflammatory medication, and has used every version of SYSTANE tears. She told me, “Since I started using the new tears, my eyes feel better, and it lasts. I’m not using my prescription drops as often.” As a result, we came up with a new strategy to manage her condition: 1) Use SYSTANE COMPLETE at least 2 to 4 times a day; 2) If a flare-up occurs, use prescription anti-inflammatory twice per day for a week; 3) We will monitor her every 3 months. So far, this approach is working well.
I also recommend SYSTANE COMPLETE before I refer patients for cataract or refractive surgery and when they return for evaluation. DED is missed too often before surgery—one study showed that 22.1% of cataract patients were previously diagnosed with DED, but 80.9% actually had moderate to severe DED15—so I am very vigilant. My contact lens patients use SYSTANE COMPLETE as well, instilling drops before and/or after insertion to protect the ocular surface (and prevent dropout). It’s possible for DED to be present in any patients, regardless of why they are in my office, so it certainly helps to know that a dry eye drop is designed to provide symptom relief for every major type of dry eye.4-6
SYSTANE is a trademark of Alcon. © Alcon 2018. All other brand/product names are the trademarks of their respective owners.
© 2018 Novartis 9/18 US-SYS-18-E-2048
- American Academy of Ophthalmology. Eye Health Statistics. Available at: https://www.aao.org/newsroom/eye-health-statistics. Accessed July 13, 2018.
- Nielsen Homescan Ailment Panel, Annual Survey 2017, Quintiles IMS data.
- Lemp MA et al. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea. 2012;31(5):472-478.
- Ketelson H, Rangarajan R. Pre-clinical evaluation of a novel phospholipid nanoemulsion based lubricant eye drops. Invest Ophthalmol Vis Sci. 2017;58(8):3929.
- Data on file. Alcon; 2017.
- Craig J, Nichols K, Akpek E, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017;15:276e283.
- Benelli U. Systane lubricant eye drops in the management of ocular dryness. Clin Ophthalmol. 2011;5:783–790.
- Korb D, Blackie C, Meadows D, Christensen M, Tudor M. Evaluation of extended tear stability by two emulsion based artificial tears. Poster presented at: 6th International Conference of the Tear Film and Ocular Surface: Basic Science and Clinical Relevance; September 22-25, 2010; Florence, Italy.
- Lane S, Paugh JR, Webb JR, Christensen MT. An evaluation of the in vivo retention time of a novel artificial tear as compared to a placebo control. Invest Ophthalmol Vis Sci. 2009;50(13):4679.
- Torkildsen G. The effects of lubricant eye drops on visual function as measured by the Inter-blink interval Visual Acuity Decay test. Clin Ophthalmol. 2009;3:501-506.
- Moon SW, Hwang JH, Chung SH, Nam KH. The impact of artificial tears containing hydroxypropyl guar on mucous layer. Cornea. 2010;29(12):1430-1435.
- Davitt, WF, Bloomenstein M, Christensen M, Martin AE. Efficacy in patients with dry eye after treatment with a new lubricant eye drop formulation. J Ocul Pharmacol Ther. 2010;26(4):347-353.
- Willcox MDP, Argueso P, Georgiev GA, et al. TFOS DEWS II tear film report. Ocul Surf. 2017;15:366-403.
- Jones L, Downie LE, Korb D, et al. TFOS DEWS II management and therapy report. Ocul Surf. 2017;15:575-628.
- Trattler WB, Majmudar PA, Donnenfeld ED, McDonald MB, Stonecipher KG, Goldberg DF. The Prospective Health Assessment of Cataract Patients’ Ocular Surface (PHACO) study: the effect of dry eye. Clin Ophthalmol. 2017;7(11):1423-1430.


