Despite advances in scleral lens technology, anterior surface wetting issues continue to plague some patients (Figure). Even though these patients may have seen dramatic improvements in their vision, milky or hazy vision leads them leave their scleral lenses in their case to collect dust (or at least to soak in an appropriate solution). Scleral lens fitters can help these patients with a few tips and tricks. Implementing some of this tips into your examinations and patient education can save you chair time and reduce fogging complications.
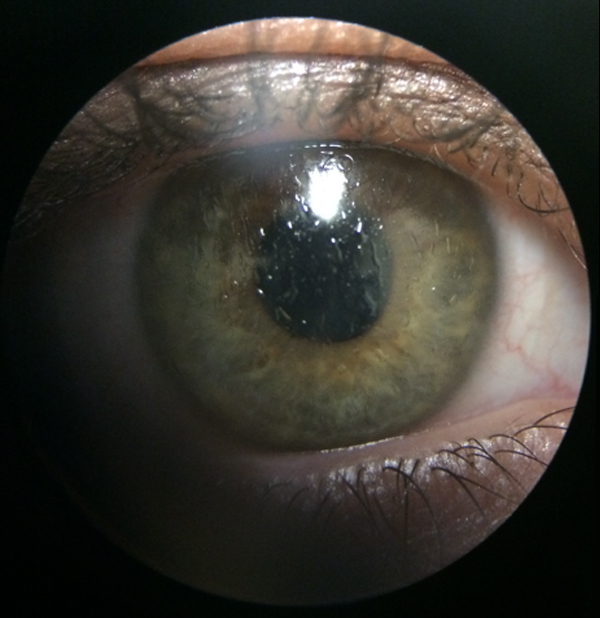
Figure. Wetting issues can result in discomfort and increase the risk that a patient will discontinue scleral lens wear.
LENS WETTING ISSUES
Surface wetting refers to the ability of liquid to spread across a surface and it often described alongside its wetting angle. A contact lens material with a low wetting angle has moisture more evenly dispersed and with fewer dry spots than materials with higher wetting angles. Gas permeable (GP) lens materials start off hydrophobic by nature, and any exposed silicone prevents lenses from properly wetting; it is often the surface treatments and coatings that give GP materials the ability to stay moist on the eye. Poor scleral lens wetting causes decreased quality of vision, decreased comfort, and results in increased chair time, more patient visits, and higher overall costs for both patient and clinician.
OCULAR SURFACE ISSUES
Aside from materials and coatings on the lens, scleral lens wettability also depends on the stability of the ocular surface. Poor tear quality can be a major factor in wetting, particularly for patients with ocular rosacea, meibomian gland dysfunction (MGD), Sjögren syndrome, or graft-vs-host disease. Manual expression of meibomian glands allows clinician to assess the quality of a patient’s meibum, which may be a factor even in patients not diagnosed with MGD. Patients using poor quality makeup products and oil-containing skin care products are also at risk of disruption of the ocular surface.
TROUBLESHOOTING: A THREE-STEP APPROACH
Clinicians who seek to improve surface wetting in their scleral lens patients should pay attention to three issues: ocular stability, materials and coatings, and patients’ at home maintenance.
Ocular Stability
Evaluation of the ocular surface and eyelids is critical in addressing wetting issues in a scleral lens patient. Use of artificial tears with surfactants can reduce surface tension and help to increase the lubricity of the lens. However, some patients may need more aggressive treatment regiments such as lifitegrast ophthalmic solution 5% (»Xiidra, Shire), cyclosporine ophthalmic emulsion 0.05% (»Restasis, Allergan) or punctal plugs. Lid margins need to be examined for blepharitis and the presence of Demodex mites and, if needed, treated in the office with electromechanical lid margin debridement (»BlephEx, Rysurg) or at home with prescription eyelid scrubs such as Avenova (NovaBay Pharmaceuticals).
Thoroughly identifying and pretreating issues during the fitting process can reduce surface wetting complications.
Materials and Coatings
Troubleshooting should include an assessment of scleral lens materials and coatings. There are a wide variety of GP materials available for scleral lenses with many different characteristics. It is important to remember that the oxygen permeability (Dk) values are only part of the scleral lens surface story. Carefully choose material with a balance of adequate Dk and low wetting angles to improve the surface of the lens. Some common materials and their wetting angles and Dk values are listed in the table.
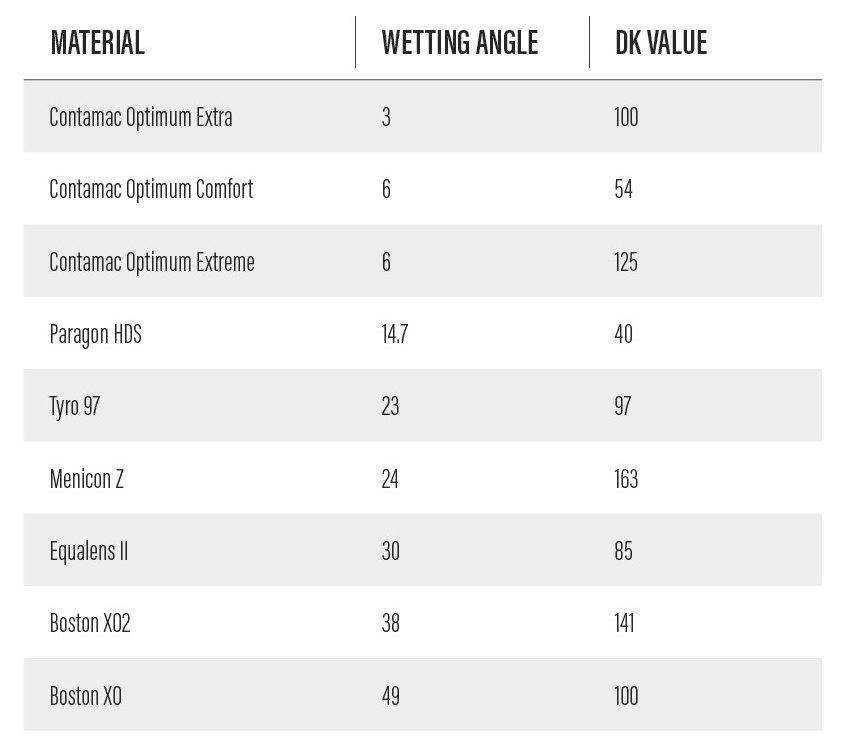
Table. Wetting angles and Dk values for various scleral lens materials. Items are in ascending order of wetting angle.
Plasma coating and polyethylene glycol coating (hydraPEG, Tangible) can also be added to the surface of the lens to improve wettability. Plasma coating is a cleaning treatment of the GP material that enable it to interact better with the water in the tears. Polyethylene glycol (PEG) coating is a layer bonded to the GP material but the length of time it lasts can vary by patient. Keep in mind that both plasma treating and hydraPEG coatings can be affected by polish and abrasive cleaners.
Maintenance
Optometrists treating a dissatisfied scleral lens patient should evaluate everything that comes in contact with that patient’s lenses. This includes contact lens solutions, cleaners, plungers, oils on the hands, and makeup and skin care products used around the eyes.
Some patients may be inclined to select a solution from their local drug store based on price or convenience. Make it clear to your patients that the solution you prescribed was chosen with their health, safety, and convenience in mind, and that use of an appropriate solutions system may prevent them from encountering wetting issues. A discussion about choosing makeup and skin care products without oils or paraben waxes can also be helpful, as these oils and waxes may interfere with the material surface.
Patients with midday fogging can use a small amount of conditioning solution or rewetting drops applied to a cotton swab or small plunger tip to act as a windshield wiper to the front surface of the lens.
SOLVE THIS PROBLEM!
Surface wetting issues can affect patients’ overall wearing experiences and can be just as disruptive as an improper fit. Do not be afraid to delve into how patients care for their lenses and their eyes while at home. The easiest solution may be grounded in the simple matter of proper lens maintenance.







