
A number of trends are converging to increase the demand for eye care services. The population 65 years and older is growing at four to five times the rate of overall population growth (Figure 1), meaning that a growing proportion of the US population is in the demographic most susceptible to age-related eye diseases, including cataracts, macular degeneration, diabetic retinopathy, and glaucoma.
Despite the increasing demand, the number of ophthalmology residency spots is not expected to increase any time soon. In fact, the number of practicing ophthalmologists will actually decline as retirement of older doctors exceeds the number of new entrants to the field. All told, the Association of American Medical Colleges estimates that the United States will have a shortage of more than 25,000 surgical specialists, including ophthalmologists, by 2025 (Figure 2).1
The use of optometrists as collaborative partners in the delivery of surgical eye care will therefore be increasingly important in the future. The new generation of optometrists is well aware that surgical and medical collaborative eye care will be an increasing part of their practice as they face competition from online spectacle and contact lens suppliers and decreasing vision wear profits.
The challenges ahead provide opportunities for both optometrists and ophthalmologists to overcome their biases and work together. At Atlantis Eyecare, we are doing this through active cooperative management with outside optometrists as well as by integrating optometrists into our in-house research department.
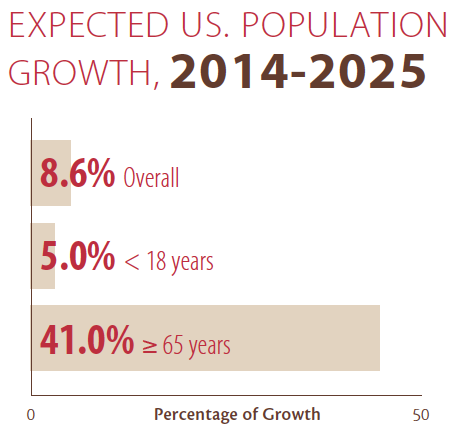
Figure 1. Per-capita consumption of health care services, including age-related eye care, will be driven by the increase in the senior (≥ 65 years) age group.1
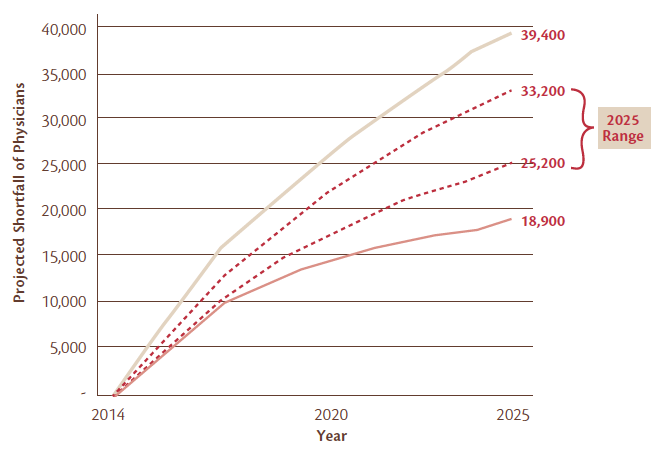
Figure 2. Projected surgical physician shortfall range, 2014-2025. Ranges are based on varying estimates for supply and demand that take into account changes in the US health insurance system, retirement rates, and other factors.1 The top dotted line represents the 75th percentile, and the bottom dotted line represents the 25th percentile.
CONTINUING EDUCATION IS KEY
We provide continuing education for in-house staff and for community optometric partners. We invite optometrists into our operating rooms and clinics to get a better understanding of screening procedures, surgical outcomes, new technologies, follow-up expectations, and more.
This is particularly important with collaborative care for cataract surgery patients. Compared with LASIK candidates, cataract patients are older, have more comorbidities, and require much more complex decision-making. For example, in a patient with ocular surface disease, we might want to postpone surgery in order to address those issues, or we might want to accelerate surgery in a patient with glaucoma in order to reduce intraocular pressure.
The IOLs we implant have also been changing rapidly. Some community optometrists outside our practice have a negative opinion of premium IOLs as a class, perhaps due to earlier experiences with presbyopia-correcting lenses. These practitioners tend to recommend against these options when counseling their patients. It will take time, but we must put in the effort now to engage with these doctors and tell them about new technologies such as laser-assisted cataract surgery and extended depth of focus IOLs, both of which I think can help to overcome their objections.
Of course, no matter what their optometrists recommend, cataract patients still want to and deserve to personally meet their surgeon and hear directly from that surgeon what he or she recommends. We offer patients that personal connection in a no-pressure environment. We use lots of audiovisual aids—from commercially available animations that illustrate lens optics to video testimonials from patients at different stages of their postoperative journey—to set patients up to have a comfortable experience.
CLINICAL TRIALS
We have a strong interest in being involved in innovative new technologies, so, about 4 years ago, we started a clinical studies profit center at Atlantis Eyecare. We are now participating in clinical trials investigating toric IOLs, sustained-release technology for glaucoma drugs, and new medications for dry eye and macular degeneration. We are also actively involved in diabetic retinopathy research as an investigator site for the Diabetic Retinopathy Clinical Research Network, or DRCR.net.
Today, our research department is financially successful for the practice, and its presence has helped to build our reputation in the community. The best part is that it helps our patients gain early access to new technologies.
A survey recently conducted by Research!America, a nonprofit public education alliance that represents industry, universities, and health-related nonprofit associations and advocacy groups, found that patients believe their doctors are reliable sources for clinical trial information. Most respondents (86%) said their health care provider should discuss clinical trial opportunities as part of their standard of care, although 74% said that their doctors had never discussed medical research with them (Figure 3). Further, 90% of respondents said they believe that clinical trials are important to advancing science.2
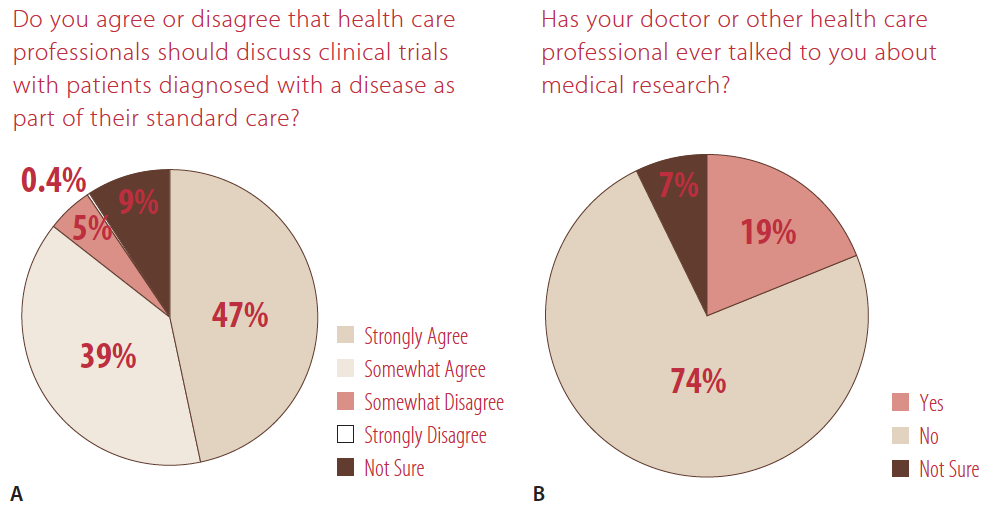
Figure 3. In a survey of US adults by Zogby Analytics and Research!America, 86% of respondents said they want their doctors to discuss clinical trials with them (A), but 74% say their doctors have never talked to them about medical research.2
RAMPING UP THE RESEARCH
I consider involvement in clinical trials a service to both the eye care community and our local community, and it has been a great experience for those of us in the practice to be able to be stay on the cutting edge and be directly engaged in the evolution of new technologies.
Initially, however, there was not much profit in our proposed clinical studies profit center. It has taken time to get established and hire the right staff. We started with phase 4 (postmarketing) studies in anterior segment surgery, then gradually expanded to glaucoma and retina. We also started participating in the more rigorous phase 3 trials that are conducted to support approval of a new drug or device.
Particularly for phase 3 studies, there are strict standards for patient enrollment, masking, data collection, and data management. The optometrists in our practice are essential in all of these areas. They manage the enrollment process and, for some studies, serve as subinvestigators. In some cases, optometrists serve as clinical coordinators, but in our large, multioffice practice, we also needed a highly skilled optometrist to manage clinical coordinators at each location.
The optometrists involved in these projects also define and oversee data entry requirements. Training staff members on how to correctly record postoperative refractions and knowing when to investigate anomalies in the data can make all the difference between junk and valid scientific insight. Data management is the foundation for everything we learn from clinical trials.
CONCLUSION
The future is bright in terms of the new technologies that we can offer patients to correct their vision and treat their diseases. Innovative practices must embrace not only these new technologies, but also new ways of practicing in order to continue to deliver care effectively and efficiently. One of the ways to achieve these aims is by incorporating collaborative care into our practice models, making full use of the skill sets of our optometric colleagues.
- The complexities of physician supply and demand: projections from 2014 to 2025: 2016 update. Association of American Medical Colleges. April 5, 2016. https://www.aamc.org/download/458082/data/2016_complexities_of_supply_and_demand_projections.pdf. Accessed August 30, 2017.
- Public perception of clinical trials. Research!America. July, 2017. http://www.researchamerica.org/sites/default/files/July2017ClinicalResearchSurveyPressReleaseDeck_0.pdf. Accessed August 30, 2017.

