As someone who works in a hospital setting and previously worked in a tertiary care ophthalmology practice, I have seen my share of complex cases. For 15 of my 17 years in the profession of optometry, I was on primary call several weeks per year for the practice. I have encountered uncountable after-hours calls and emergency patients. I was fortunate in that I always had a surgical backup (usually the institution’s cornea fellow, but occasionally one of the partners). If a case arose that was beyond my comfort level or scope, I had an immediate contact point no matter the time of day or night.
As much as I tried to manage nearly everything I could, invariably there were cases in which I was thankful to pass along the patient to my surgical partner to facilitate the best outcome. Time is often an important factor in these cases, and it is imperative that the patient is handed off in a timely manner for more involved care. Following are five such scenarios.
RETROBULBAR HEMORRHAGE
This is an uncommon but emergent scenario. Retrobulbar hemorrhage typically presents following trauma or eyelid or orbital surgery; more rarely, they can present due to a vascular malformation or secondary to anticoagulant use. Patients commonly present within 24 hours of the inciting event. Symptoms include severe pain, sudden onset proptosis, vision loss, restricted extraocular muscle movement, and subconjunctival hemorrhage.
The hemorrhage behind the globe creates an orbital compartment syndrome, and the combination of stress on the optic nerve, altered blood flow, and perfusion to the nerve puts the patient at high risk for vision loss. Treatment consists of a lateral canthotomy and cantholysis to evacuate the blood and relieve the pressure on the nerve.
OPEN GLOBE INJURY
Any patient who presents following trauma to the eye should be evaluated for an open globe injury. This includes patients who have recently undergone surgery, patients with surgical wounds that have not been closed by suture (such as after sutureless cataract surgery), or patients with surgical entry wounds who have had sutures recently removed. Standard examination should be performed by taking a careful history to determine the nature of the injury, checking IOP, and performing a Seidel test.
If a conjunctival penetrating injury is suspected, significant chemosis surrounding the entry site is another important clue. Patients with open globe injuries are at risk for vision-threatening complications including endophthalmitis and suprachoroidal hemorrhage. Careful examination for any intraocular foreign body should be made, and an attempt to close the wound should be made promptly by the surgeon on site.
ORBITAL CELLULITIS
Although orbital cellulitis is rarely encountered, it is important that clinicians be able to recognize and refer this condition. Differentiation of orbital cellulitis from preseptal cellulitis can be made through several differentiating factors. Evaluating extraocular motilities is important as they are restricted in orbital cellulits but not in preseptal cellulitis (Figure). Visual acuity is often reduced in patients with orbital cellulitis, and the presence of a relative afferent pupillary defect may indicate the presence of orbital cellulitis. The lids may be so swollen that they can be difficult to open, and proptosis may be present. These patients are usually quite sick, and they require immediate intravenous antibiotics.
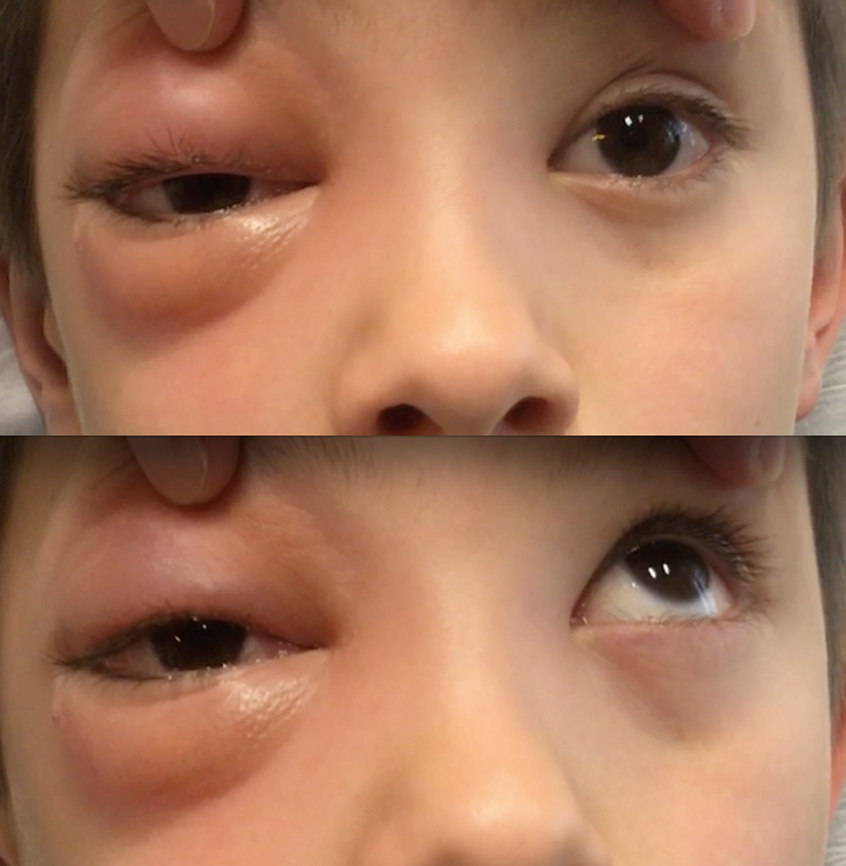
Figure. A pediatric patient with orbital cellulitis (top). Limited extraocular motility was noted upon examination (bottom). Photo credit: Cullen Ryburn, MD.
RETINAL DETACHMENT
Retinal detachments present a scenario in which prompt referral may make a significant difference in final visual outcome, particularly if the detachment is superior. During triage, the optometrist preparing for referral should note the specific location of the detachment and the time the patient last ingested food and water. These details can help the retinal surgery team prepare for examination and scheduling of surgery.
ENDOPHTHALMITIS
Infection inside the eye is very serious. Any suspicion of infection within the globe should be referred for examination and culture of the aqueous or vitreous. The seminal Endophthalmitis Vitrectomy Study found that 94% of patients reported blurred vision and up to 25% of patients did not report any pain.1 These statistics should be kept in mind during examination.
Patients at high risk for endophthalmitis are those in the first 2 weeks after surgery and those who have sustained trauma or open globe injuries. Patients at elevated risk for endophthalmitis include those who have undergone penetrating glaucoma filtering surgery, such as trabeculectomy and (less commonly) tube shunt implantation. Patients with decreased vision and layered hypopyon with more inflammation (cell and flare) than would normally be expected should be evaluated promptly.
REFERRAL MAY SAVE VISION
Optometric collaboration with ophthalmology includes knowing when an appropriate, immediate referral to a surgical colleague is the right call to treat an emergent presenting condition. In the examples described above, prompt referral could be sight-saving, eye-saving, or at the very least can increase the likelihood of a good visual outcome for the patient.
- [No author listed.] Results of the Endophthalmitis Vitrectomy Study: a randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Endophthalmitis Vitrectomy Study Group. Arch Ophthalmol. 1995;113(12):1479-1496.






